Arthritis Osteoarthritis
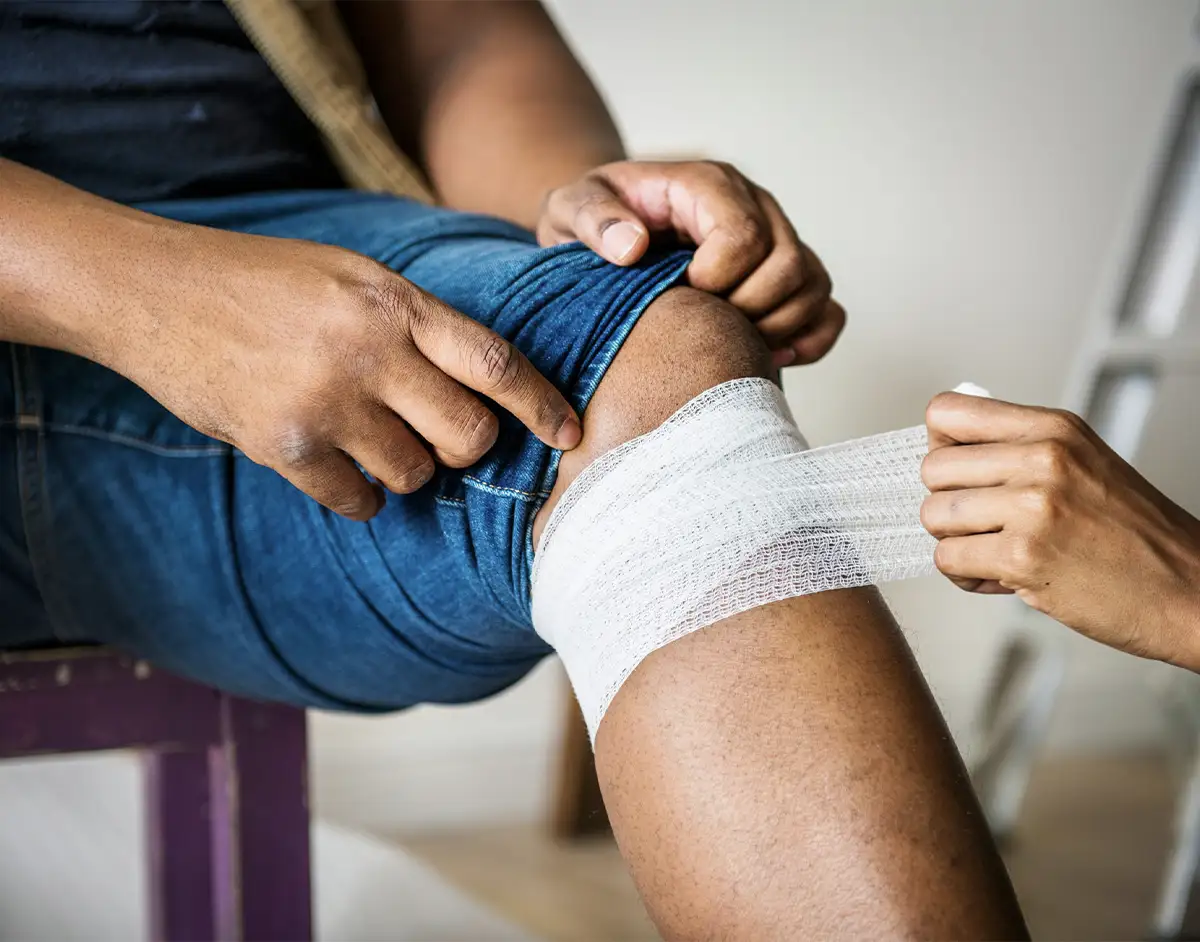
Arthritis, or degenerative osteoarthritis, of the knee is caused by long term wear and tear to the cartilage that naturally cushions the knee joint. This causes the bones in the joint to rub together and cause permanent damage.
In some cases, arthritis can also be triggered – or made worse – by a knee injury that damages a particular area – this is known as ‘traumatic osteoarthritis’ and can often happen as a result of sporting activities.
QUICK LINKS
What can increase my risk of knee arthritis?
Although knee arthritis can affect anyone, it’s more likely to develop if your parents or siblings have had the condition or if you’ve previously had an injury or operation on your knee. It’s also more likely to be a problem if you:
- Have another joint disease such as rheumatoid arthritis or gout
- Carry out heavy manual work such as farming
- Are over 40
- Are female
- Are overweight or obese
- Take part in sports such as running, athletics, football or rugby which result in long term wear and tear on the joints
Knee arthritis
These include:
- Pain, swelling and stiffness in the knee
- A sensation of creaking or grinding in the joint when it moves
- Difficulty carrying out everyday activities such as walking, climbing stairs, bending, squatting and kneeling
- Knee instability (when your knee feels unstable and/or gives way)
- The knee catching or locking when you bend or straighten it
As arthritis develops, symptoms become worse. In some cases, walking may become more difficult and you may also be in pain at night.
Your consultant will discuss your symptoms with you and examine your knee to check for tenderness, stiffness, swelling and any difficulties with movement. In most cases, they will arrange for you to have an X-ray to confirm the diagnosis of arthritis. They may also arrange for you to have a magnetic resonance imaging (MRI) scan to show any damage to the soft tissue (cartilage, tendons and muscles) in your knee.
Treatment depends on a number of factors including how much the arthritis is affecting your everyday life and activities, as well as how worn the knee joint has become.
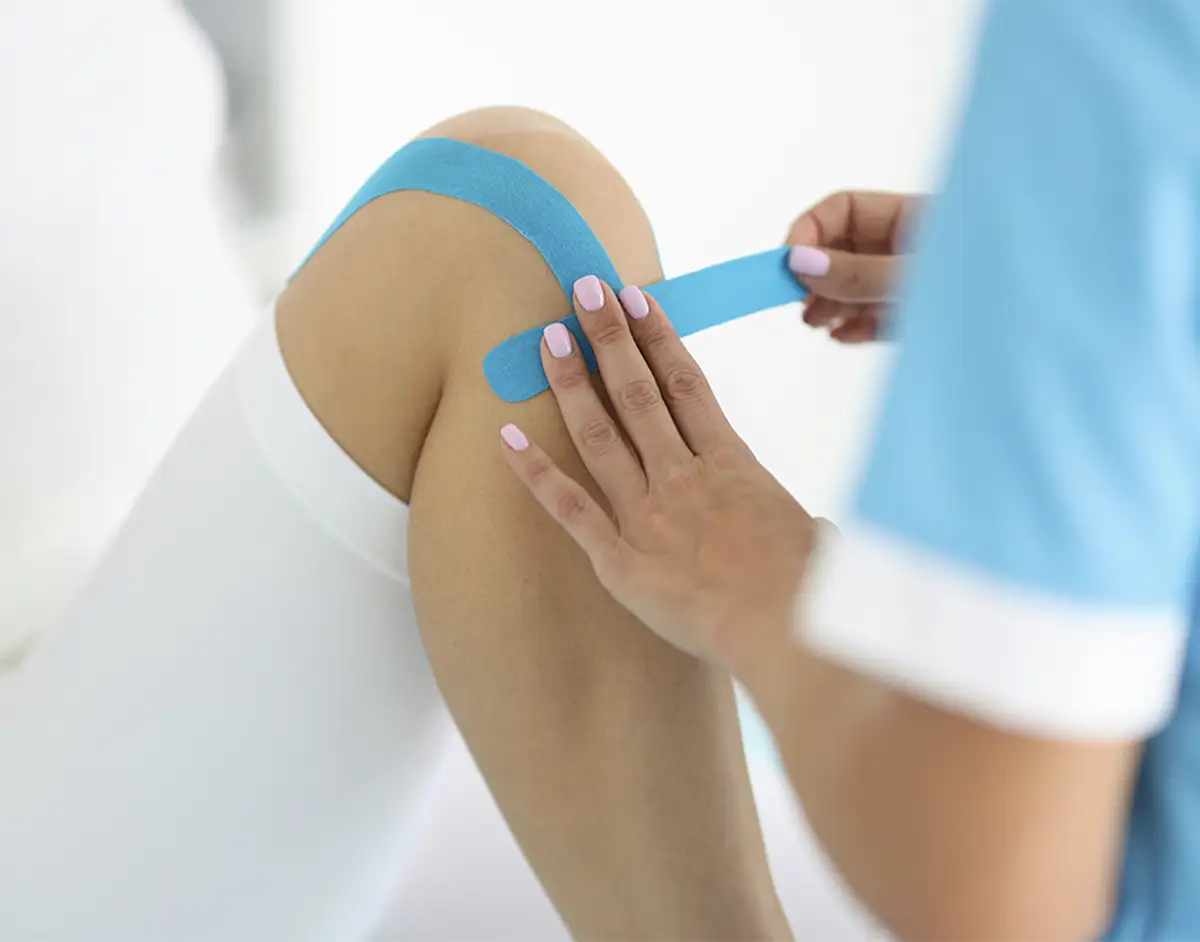
- Non-surgical treatment includes: making lifestyle changes along with having physiotherapy and taking painkillers (as prescribed by your doctor). In some cases, this can be enough to reduce your symptoms. You may also be offered injections to reduce inflammation in the joint, as well as a brace to support the knee joint
- Surgical options include knee realignment surgery (osteotomy), partial or total knee replacement surgery or knee joint distraction. In some cases, you may also be offered adipose tissue therapy